
An estimated 27 million Americans suffer from thyroid-related illness, the majority of them are women. Many of the patients I see in my practice have been “ill diagnosed” or sub-optimally treated. In today’s blog I will review basic thyroid physiology and function.
What is your thyroid gland and what does it do?
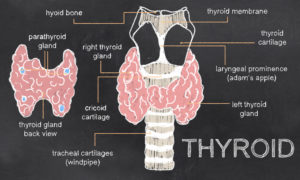
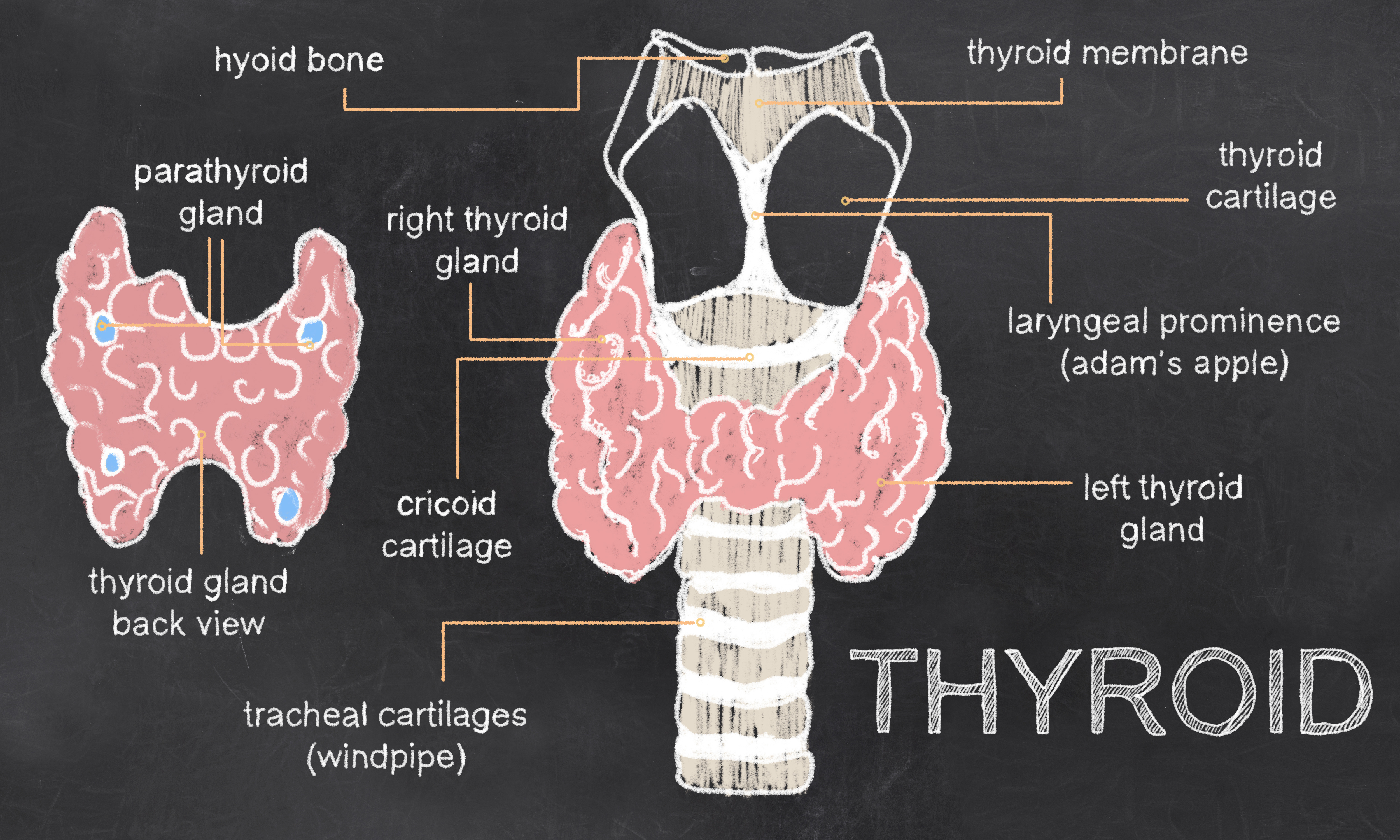
The thyroid is a butterfly shaped endocrine gland located in the front of your neck near your Adam’s apple. The thyroid has a key role in regulating metabolism, growth and development and bodily functions. Your thyroid makes several primary hormones including T4 and T3.
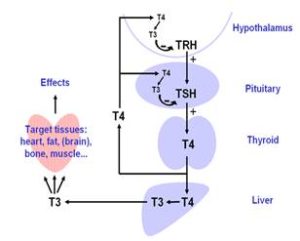
The pituitary gland releases TSH (thyroid stimulating hormone) to help regulate the balance of thyroid hormones. So when your thyroid hormone levels are too low, it sends a signal to the hypothalamus in your brain to release TRH (thyroid releasing hormone), which in turn stimulates your pituitary to release more TSH,with the ultimate goal of stimulating more T3 and T4 production. Conversely, when your thyroid is making too much thyroid hormone, a signal is sent back to the pituitary gland to suppress thyroid hormone production. This typically occurs with hyperthyroidism or an overactive thyroid gland. In this situation, the TSH is typically low.
Conversion of T4 into T3
image source: healyourselfathome.com
Your thyroid primarily secretes T4. Of the total thyroid hormone secreted, T3 is only accounts for approximately 7 – 10%. Since the body can only use T3, it must convert T4 into T3 by removing one molecule of iodine. This conversion occurs in the liver, the gastrointestinal tract, and a variety of other cells in your body. Twenty percent of T4 to T3 conversion occurs in the intestines, but only in the presence of healthy gut bacteria.
Thyroid hormones are bound to proteins. Only the hormone that becomes unattached or free is metabolically active. The binding of thyroid hormones can be impacted by a variety of factors such as pregnancy, illness, estrogen replacement and many medications. So for example,estrogen replacement therapy increases the binding of thyroid hormone, resulting in less free or metabolically active thyroid hormone. In this case, a woman’s lab work may show a normal or slightly low TSH, a normal or high T4 and a normal or low Free T4. So the point is, measuring total T4 in a women with a thyroid hormone binding abnormality is not as useful as measuring the amount of free thyroid hormone.
Is measuring TSH enough?
As we discussed earlier, TSH is the stimulating hormone released by the pituitary gland. Measuring TSH is the most common way to assess thyroid function. When TSH is high, it is assumed that the thyroid gland is not working properly and medication is needed to boost thyroid performance. This assumes that the individual has an intact hypothalamic-pituitary-thyroid axis and overlooks numerous other factors that can impact thyroid function and balance such as thyroid binding abnormalities, pituitary dysfunction and underlying autoimmune thyroid disease. In addition, the current reference range for TSH has a wide range and can often miss sub-clinical thyroid dysfunction.
Stay tuned for my series of upcoming posts which will discuss more on Getting to the Root Cause of Thyroid Imbalance.